Pregnancy Blog
Blurry Vision While Pregnant: When It’s Normal—and When It’s Not
Question: I’m in my fifth month of pregnancy, and my eyesight seems to be getting worse. My contacts don’t fit quite right anymore. Am I just imagining this? Answer: You are absolutely not imagining it! Experiencing blurry vision while pregnant is actually very...
Difference Between Gas Bubbles and Baby Moving—And When to Expect Those First Kicks
One of the most talked-about and confusing experiences of pregnancy is trying to figure out whether what you're feeling in your belly is your baby moving or just gas. You're not alone if you find yourself second-guessing every flutter and bubble. Here's everything you...
Exhaustion During Pregnancy: Why It Happens And 7 Ways to Feel Better
Tiredness, exhaustion, fatigue: whatever you call it, exhaustion during pregnancy can be challenging. Many pregnant women report that it becomes difficult to get up for work each day, and some feel like they're simply dragging from morning until bedtime. While this...
Why Am I Having So Many Braxton-Hicks Contractions?
If you’re pregnant and feeling your belly tighten up throughout the day, you might be experiencing something called Braxton-Hicks contractions. These are “practice contractions” that many pregnant women feel, especially in the second and third trimesters. Some...
Shampoo and Conditioner for Pregnancy: What You Need to Know
When you're pregnant, you become more aware of everything you put on and in your body, and for good reason. While many shampoos and conditioners line store shelves with promises of healthy, beautiful hair, not all of them are created equal when it comes to pregnancy...
Can You Take Antidepressants While Pregnant?
If you're feeling depressed during pregnancy, you're not alone. Studies estimate that approximately 9-16% of pregnant women experience depression, with some research suggesting rates as high as 20%. That means potentially two out of three pregnant women in America...
5 Pregnancy-Safe Teas You’ll Love
When pregnant, knowing what’s safe to eat and drink can be challenging. If you’re craving a cup of tea, know there are safe teas to drink while pregnant. Plus, drinking tea is smarter during pregnancy than caffeinated drinks. Most healthcare professionals advise that...
The Best Pregnancy Safe Foundation for Every Budget
There are a lot of things to take into account when you're pregnant. Besides physical changes, you also have to be mindful of what you put on your body, including everything from your sunscreen, shampoo, face wash, and more. So while you may already be enjoying that...
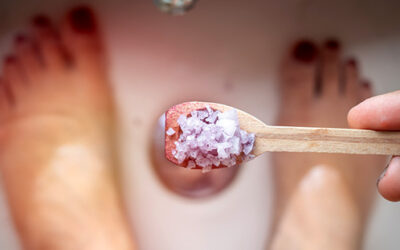
Is an Epsom Salt Bath During Pregnancy Safe? Everything You Need to Know
Epsom salt baths feel divine when you're pregnant! This natural remedy for aches and pains is completely safe for pregnant women. You use Epsom salt by putting it into your bathwater and then taking a long, luxurious bath. Many athletes swear by Epsom salt baths for...
Pregnant While on Birth Control? What You Need to Know
"I got pregnant while on birth control pills. I kept taking them for about a month because I had no clue I was pregnant. Will this affect my baby?" Don't panic: you're not alone. Getting pregnant while on birth control pills happens more often than you might...
The Truth About High Altitudes While Pregnant (It’s Complicated)
When you're pregnant and planning to travel, there are a lot of things to think about, especially when it comes to high altitude. So you're expecting and dreaming of those Instagram-worthy mountain views? Hold up – before you start packing your hiking boots, let's...
Is Soft Serve Ice Cream Safe During Pregnancy?
One of the best parts of being pregnant is that no one’s judging you as you thoroughly enjoy your dinner (and some ice cream.) Ice cream is a pretty typical pregnancy craving — with or without pickles. Feeling tempted to devour the entire pint in one sitting? The...
How to Perform the Most Popular Prenatal Yoga Poses
Staying active during pregnancy is essential, as is making time for rest. Practicing prenatal yoga poses allows you to connect with your body while building strength, improving flexibility, and enhancing balance. These movements can support both mental and...
Do Contractions Make You Fart?
Your growing baby can affect your digestive system. To start, there's morning sickness. Then, your hormones disturb the digestive process, and your baby grows larger, moving your organs along the way. A hormone called prostaglandin gets your body ready for...
Can I Have Chinese Food While Pregnant?
Navigating a restaurant menu while pregnant can be challenging. You might find yourself either extremely hungry or feeling nauseous. Many women have wondered, "Can I have Chinese food while pregnant?" It's important to be mindful of foods and drinks to avoid...
Driving While Pregnant: What You Need to Know for a Safe Journey
With all the restrictions placed on pregnancy, it's natural to wonder if you're still allowed to enjoy everyday activities—like taking a shower, strolling along the beach, or driving a car. Is it safe to be driving while pregnant? In most cases, the answer is a...
Your Ultimate Guide to Safe and Effective Pregnancy Exercises at Home
Pregnancy is an incredible journey, but it can be tough on your body. That’s why taking care of yourself is so important—not just for you, but for your little one too. One of the best ways to stay healthy during this time is by staying active through pregnancy...
Navigating the News: How to Tell Your Parents You’re Pregnant as a Teen
“I am 16 and pregnant. My boyfriend is 17 and the only person who knows about it. I’m 8 weeks along and haven’t gone to a doctor yet. I am so scared to tell anyone, especially my parents. I dread telling them because I come from a well-educated family of doctors and...
How to Get Ready for Labor
Having a baby is a major life event, so feeling overwhelmed is completely normal. There is a lot to learn and decide, but preparing ahead will make your labor and delivery experience easier. You might be wondering how to get ready for labor. Your body naturally...
Forgetfulness During Pregnancy: How to Manage It
Most moms-to-be expect some of the physical symptoms of pregnancy: an expanding baby bump, morning sickness, swollen ankles, and glowing skin. But in addition to these symptoms, you probably weren’t expecting to add forgetfulness to the list of changes! But is...
What to Do After a Positive Pregnancy Test
For some, the thought of a positive pregnancy test is a long-awaited dream come true, while for others, it may come as a complete surprise. A positive pregnancy test can bring up an abundance of emotions and have you wondering what steps to take next. If you're asking...